The public health challenge of our generation is right in front of us. SARS-CoV-2 appears to be the Andromeda strain that public health workers fear to see emerging. After many years of working at the Centers for Disease Control and Prevention, I’m perplexed, and saddened, that the agency seems to be sitting on the sidelines for this pandemic and is not building on the accumulated skills and experience from its past.
Nobody dismisses the worsening crisis or its ability to deal a potentially deadly blow to health systems and economies around the world. Health care providers throughout the U.S., emulating those in other countries, are improvising protective equipment. Bandanas are the new N95 face masks. Clinicians and other providers wait days or weeks to get the results of nasal swabs collected at great risk from patients suspected to have Covid-19. From nurseries to universities, from small businesses to large corporations, nearly everybody is, or likely will soon be, quarantined, locked down, and rightfully scared.
For decades, the CDC has been at the forefront of responding quickly to new and emerging disease threats. During previous outbreaks, teams of responders have been quickly deployed in the U.S., at the request of one or more states, as well as in remote and sometimes socially unstable places at the request of foreign governments. The mission of these teams is to guide and support local, national and international public health response efforts.
In the spring of 1993, an unknown disease was detected in the Four Corners region of Colorado, Utah, Arizona, and New Mexico. A CDC team was dispatched to the area. In just a few weeks, CDC scientists had not only identified and described a new hantavirus, but they also created a diagnostic test for laboratories. By the end of 1993, patients were found in multiple states and tens of thousands of blood samples had been run in one of CDC’s laboratories.
Sign up for Daily Recap
A roundup of STAT’s top stories of the day.
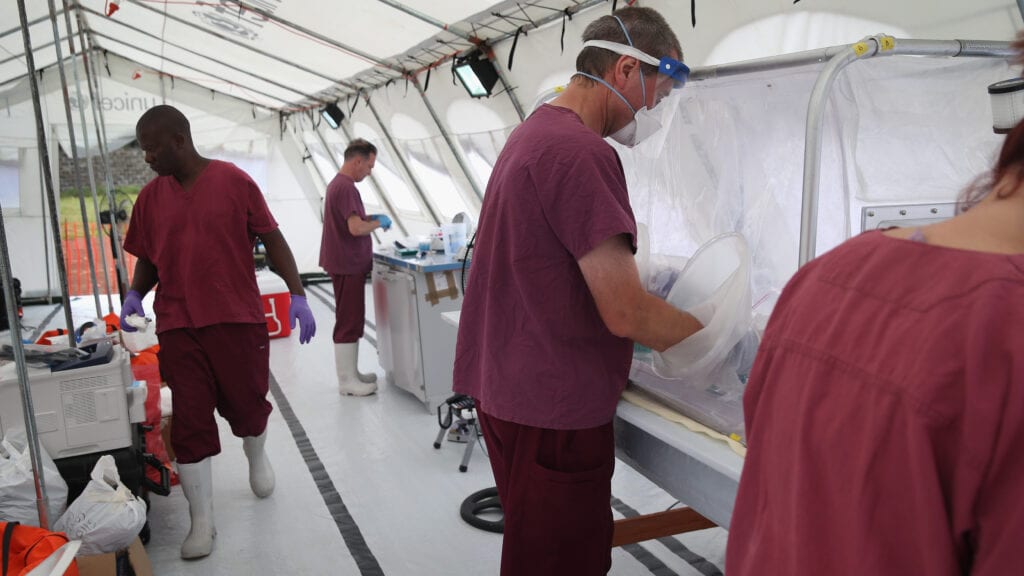
During the 2014-2016 Ebola outbreak, the CDC enlisted thousands of responders from the U.S. and various affected African countries, and staffed a laboratory first in Kenema, and then in Bo, Sierra Leone that conducted more than 16,000 Ebola tests under difficult local conditions.
advertisement
Over the decades, CDC workers developed many new diagnostic assays during emergencies to respond promptly to new or orphan diseases.
Annual funding cycles and conflicting priorities have challenged the CDC’s ability to maintain expertise and replenish human resources. New layers of bureaucracy, created in the late 2000s, fostered increased top-down regulation, slowing or blocking initiative and innovation. Productivity declined as research and clinical laboratories were saddled with strict and complicated Clinical Laboratory Improvement Amendments (CLIA) rules and an insistence on FDA-approved tests — even for tests developed and run only in CDC reference laboratories.
Each year supervisors must take mandatory leadership training courses regardless of their demonstrated skills and experience. Instead of mentoring younger generations at the bench, laboratory managers and leaders spend much of their time in the office to working on time-consuming lab-related paperwork and seeking clearer explanations of new regulations.
The CDC’s inability to respond quickly to a pandemic like Covid-19 shouldn’t come as a surprise. It was ill-prepared to develop and distribute laboratory tests, not only to state laboratories — which the CDC had done previously, albeit for rare and infrequent diseases — but also to commercial laboratories, a completely different and uncharted task.
The use of other diagnostic assays for SARS-CoV-2, including one recommended by the World Health Organization, were blocked in the U.S. by the Food and Drug Administration, pending the Emergency Use Authorization. The belated recognition by the Department of Health and Human Services and the U.S. government of the gravity of the Covid-19 outbreak resulted in new requests and rules for the Atlanta-based CDC. The inevitable politicization of the response added further challenges. The CDC is, after all, a governmental agency.
Despite these and many other challenges, numerous CDC scientists, young and old, seasoned and newly hired, have responded to the Covid-19 call. Hundreds of civil servants, Commissioned Corps officers, and contactors are staffing 24/7 the CDC’s Emergency Operations Center or are deployed in the field. The center’s coronavirus laboratory is working long hours to keep up with testing samples, reporting results, and fielding requests from everybody.
Starting this week, all “nonessential” CDC staff and those not already involved in the response were asked to prepare for an extended period of telework. This also covers a large number of laboratory personnel, most of whom can’t do the daily bench work from home. The potential impact of this on the CDC and the CDC Covid-19 response could be tremendous.
Inexplicably, offers by CDC laboratorians to volunteer for the Covid-19 response and support the coronavirus laboratory with added manpower were refused by CDC administrators, who seem incapable of understanding the dire situation occurring outside the organization’s gates, hiding behind cumbersome regulations developed for peacetime settings.
One might argue that all CDC staff are essential staff. Although many of them could or would prefer to work from home for personal reasons, laboratorians should be in the lab. Most want to help fight this pandemic, from running the current coronavirus assays to developing and testing new ones, testing virus inactivation methods, evaluating much-needed safety protocols, and adding their expertise in outbreaks and laboratory work to the response.
In a rapidly changing situation like Covid-19, scientific questions arise frequently, and only synergy between researchers will keep up with the demands.
Peace time rules and regulations are not well-adapted to an actual “war” situation, which is how many see Covid-19. These rules and regulations must be adapted by leaders who understand the reality of rapidly evolving outbreaks and the need to act expediently.
With its considerable laboratory resources, the CDC should be able to test thousands of samples every day. Confirmation from CDC labs lets clinicians and health institutions better manage the situation, instead of being forced to remain in the dark. Early detection of infection in a patient will expedite correct management, diminish the risk of transmission, allow enrollment in therapeutic clinical trials, and increase chances of survival.
This CDC surge laboratory capacity could be reduced later on when hospital and commercial laboratories will be able to take up the slack in diagnostic testing.
In these difficult times, many CDC workers are looking for leaders such as Walter Dowdle, a CDC scientist and key visionary leader. He pledged to the American people that CDC will base all of its public health decision on the highest quality scientific data, openly and objectively derived, and to place the benefits of society above the benefits of the institution.
We need — today not tomorrow — the emergence of many more such leaders within the CDC.
Pierre E. Rollin, M.D., worked for the CDC for 27 years, retiring in 2019 as epidemiology team lead of the Viral Special Pathogens branch.
This content was originally published here.